Anal cancer
What we do
The Chelsea Anogenital Neoplasia Service (CANS) is a bespoke, multidisciplinary, tertiary referral service within the North West London Cancer Alliance for patients with anal pre-cancer, otherwise known as high-grade squamous intraepithelial lesions (HSIL), previously known as AIN3. The service delivers best practice for the screening, treatment and surveillance of anal pre-cancer in all high-risk patients, with a specific focus on high-risk women.
The service is a clinical partnership between HIV and Sexual Health, Gynaecology and Colorectal teams to improve patient experience and reduce the burden of multiple care episodes for women with multizonal anogenital disease. It also focuses on clinical and community engagement to improve education on human papillomavirus (HPV) related disease.
CANS works to identify and treat anal pre-cancer in high-risk patients and reduce the number of patients presenting with late-stage anal cancer.
Objectives
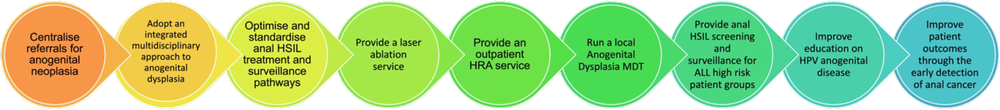
Anal cancer and HPV
The anus is where your bowel connects to the outside of your body (the bottom). Cancer here can present as:
- Pain and itching
- Bleeding or mucus discharge
- Lumps around or inside the anus
- Change in bowel habit
As many as 20% of those diagnosed with anal cancer have no symptoms at all.
Anal cancer is caused by high-risk strains of HPV. It is a rare cancer affecting 1–2 per 100,000 people each year but, in certain high-risk populations, its incidence is significantly higher and rising.
Most sexually active women and men will be infected with HPV in their lifetime—regardless of their sexual practices—and most people will clear this infection. However, some individuals are unable to do so and persistent infection with high-risk HPV can eventually cause cancerous changes in the anogenital region. Some risk factors for persistent infection are:
- Smoking
- HIV
- Cancers or precancerous lesions of the genital area (eg cervix, vulva, vagina)
- Long-term immunosuppression (eg transplant patients)
Small anal cancers, less than 2cm in size, can be surgically excised, while larger cancers may require chemotherapy and radiotherapy or, ultimately, surgery.
Like other HPV-driven cancers—such as vulval, vaginal and cervical cancer—anal cancer also has its own pre-cancerous precursor called anal squamous intraepithelial lesion (HSIL). The ANCHOR study published in Jun 2022 was the first to demonstrate that the treatment of anal pre-cancer significantly reduces disease progression to invasive anal cancer by as much as 57%. These findings have influenced how we approach anal pre-cancerous lesions and has highlighted the need for early treatment and close surveillance.
For clinicians
Our team
The Anogenital Dysplasia multidisciplinary team includes clinical experts from our HIV and Sexual Health, Colorectal and Gynaecology services. The team also has a specialist advanced nurse practitioner and administrative coordinators to manage your care. Our team of experts will provide you with information and coordinate your care pathway.
Together we manage patients at high risk of anal cancer such as women with multizonal anogenital dysplasia, immunosuppressed patients and patients living with HIV. We run regular multidisciplinary anogenital dysplasia meetings, operative lists dedicated to the treatment of anogenital pre-cancer and services such as high resolution anoscopy (for the diagnosis and surveillance of anal pre-cancer) and laser ablation of anogenital precancer (for the treatment of anogenital pre-cancer).
Consultants
- Miss Sarah Mills, General and Colorectal Surgery
- Miss Ann-Marie Howell, General and Colorectal Surgery
- Miss Elaine Palmer, Obstetrics and Gynaecology
- Miss Helen Staley, Obstetrics and Gynaecology
- Dr Christopher Scott, HIV and Sexual Health Medicine
Advanced Nurse Practitioner
- Marie-Francoise Jakarasi
Administrators
- Fadumo Ismail
Patient journey
Patients are referred to the CANS service via tertiary referrals from other hospitals and internal in-trust referrals. We do not accept GP referrals or self-referrals to the service.
Once a referral is made and accepted by one of our clinicians, patients are offered an outpatient appointment. Confirmation of appointment date and time along with an online questionnaire will be sent to the patient one week before their first appointment.
During the appointment, the doctor will ask the patient questions about their medical history and decide if a biopsy is necessary following assessment. If cases are unsuitable for referral to the CANS service, we will provide advice and guidance on management and when to re-refer.
Three to four weeks after the first appointment, the doctor will contact the patient with results and decide on possible treatments or further follow-up.
The patient may be:
- Discharged if results are unremarkable and there is no need to return
- Put on surveillance and reviewed in intervals of 3–6 months
- Offered treatment which the doctor will explain in detail to the patient
A letter will be sent to the patient’s GP and/or referring hospital with the patient’s outcome.
mASCARA registry
mASCARA (Multinational Anal Squamous Cell Carcinoma Registry and Audit) is a voluntary research database for patients with anal squamous cell carcinoma (SCC) and anal squamous intraepithelial lesions (SIL). We will ask for your consent to take part in this registry.
We create databases of rare cancers such as anal squamous cell carcinomas so that we can study them in greater depth with larger patient numbers. It is difficult for us to produce high quality research for rare cancers unless we can recruit and study many patients. We hope that including your data, along with other patients, and collaborating with research teams internationally will provide answers to important research questions and improve care.
If you agree to take part, your clinical data will be submitted to the registry—but only your local clinical team will be able to see your personal data. Anyone else accessing the database will not be able to personally identify you as your data will be held anonymously.
For more information about this study, please speak to your clinician.
Patient information
- Anal Cancer
- Anal Precancer
- High Resolution Anoscopy
- High Resolution Anoscopy and Laser Ablation
- HPV and HPV Vaccination
- Instructions for 5-Fluorouracil (5-FU) Cream (Efudix) application
- Instructions for the application of topical Aldara (5% Imiquimod)
Contact information
Chelsea and Westminster Hospital
Outpatient clinics
Lower Ground Floor
Treatment Centre
Ground Floor
E: chelwest.anogenitaldysplasiaservice@nhs.net
T: 07880 016577 (Advanced Nurse Practitioner)

